An
Interdisciplinary Paradigm of Mother-Child Health Needs
Azher
Hameed Qamar (www.drazher.com)
Health
coverage is an important issue that public and private healthcare organization
face while struggling to provide quality healthcare services to the targeted
population. An effective coverage is defined as “the proportion of a population
in need of a service that had a positive health outcome from the service”
(Marsh et al., 2020: e732). Standardized cascade for measuring effective
coverage as proposed by Effective Coverage Think Tank Group has seven steps
beginning from the identification of the target population and finally reaching
outcome-adjusted coverage. Outcome-adjusted coverage is the proportion of
population that receives the quality care adhering to providers instructions.
It is clearly indicated that proportion of population in need of health service
will significantly decline reaching the final stage.
As
mother-child health is one of the primary focus of the effective coverage, my
interest in this article is related to address people’s adherence to health
services in connection with their cultural context that is an interdisciplinary
construct. Marsh et al. (2020) examined the sequence of patient and health
system interaction in the ‘proposed standardized cascade for measuring
effective coverage’ and provided a useful insight into health service coverage.
It was an interesting article and I was able to recall my ethnographic
experience investigating infant care belief practices in rural Punjab a few
years ago. My findings were interesting as I explored the nexus between
healthcare beliefs and health-seeking behavior that determines the specific
health needs in the folk health care system.
Commentary
Medical
care (modern childcare practices) represents a highly technocratic model of
physical well-being. The concept of the ‘technocratic model’ was first used by
Davis-Floyd (1992) in the context of childbirth. In reproductive physiology,
Obstetrics, and Pediatrics, the reality of the human body is a technocratic
construct and human is an object. A young child (an infant) is a physically
immature human-becoming and an absolute dependent human body. An
expert-centered physiological exploration determines the planning and
implementation of a quality healthcare system for young children. A universal
conceptualization of the human body institutionalized by physicians and medical
professionals drives the ‘globalization’ of developmental goals to ensure
healthy lives across the globe. In this context a ‘numerical definition’ of the
child determines the developmental status and needs of the child following the
numerical age of the child. It is evident that the ‘quality health system’ is
apprised as a universal paradigm to measure the progress of coverage and
intervention plans and policies.
Based
on my assumptions (stated above) about the technocratic model of healthcare
services, I want to emphasize on step 6 of the proposed standardized cascade
for measuring effective coverage, that is adherence-adjusted coverage. There
are two main aspects of adherence-adjusted coverage. The first health care
service should be according to the quality-of-care standards (as prescribed in
WHO guidelines). Second adherence of the population (in need) to the service
provider’s instruction. Quality-of-care standards emphasized on (WHO, 2016);
- Women’s
positive experience of pregnancy, birth and postpartum motherhood based on
women’s values in their context
- Including
community participation and women voices in the planning, implementation,
and monitoring of the healthcare system
In
line with these recommendations for quality-of-care standards, the adherence to
provider’s instruction requires a contextualized body of instructions that
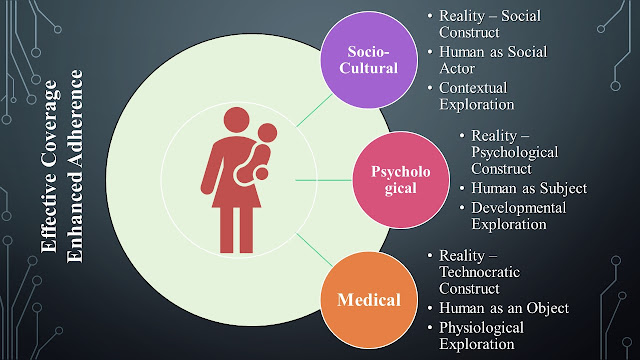
should reflect a shared understanding of the human body and health needs. Here,
we move ahead of technocratic perspective on the human body and emphasize the
socio-cultural perspective that sees human world realities as socially
constructed and mother-child health as an interdisciplinary paradigm comprised
of medical, psychological, and socio-cultural components of health needs
(figure below).
In this perspective, the quality-of-care standard as well as the provider’s instruction should be grounded in the social and cultural context. The cultural competency of the providers will enhance the adherence of the target population. This is the concern that Marsh et al. (2020) pointed out as ‘less-tangible components of quality of care’. I endorse Marsh et al. mentioning the gaps between the target population and the population who contact for their health needs. This is a major issue that must be investigated through a qualitative exploration of the underlying reasons. The socio-cultural context is multi-layered, and each layer is a layer of interconnected meanings. Addressing this gap can help to increase a culturally supported adherence.
Conclusions
Despite
the universality of physiological aspects of mother and child health,
pregnancy, birth and postpartum experiences are not universal and involve a
wide range of emotional, spiritual, and social aspects. Human health is more
than a ‘medical art’ (Farber, 2011) and human health-seeking behavior is
closely connected with their health needs and healthcare awareness. I see
medical, psychological, and socio-cultural aspects of our health-related
awareness as received, perceived, and internalized awareness respectively. An
in-depth understanding of health-seeking behavior of the target population can
be utilized to reduce the gaps between each step of the standardized cascade
discussed in the article by Marsh et al. With my ethnographic research
experience, I assume that a need-based survey may not help in improving the
healthcare system, effective coverage, and expected positive outcome; unless
health needs are not contextualized with evidence-based analysis of human
health-seeking behavior in specific socio-cultural context. Methodological
flexibility in data collection is important in this regard.
References
Davis-Floyd, R. E.
(1992). Birth as an American Rite of Passage.
Austin: University of Texas Press.
Farber, M. E. (2011). The
technocratic birthing model as seen in reality television and its impact on
young women age 18–24.
Marsh, A. D., Muzigaba, M.,
Diaz, T., Requejo, J., Jackson, D., Chou, D., … & Banerjee, A. 2020.
Effective coverage measurement in maternal, newborn, child, and adolescent
health and nutrition: progress, future prospects, and implications for quality
health systems. The Lancet Global Health, 8(5),
e730-e736.
WHO. 2016. WHO
recommendations on antenatal care for a positive pregnancy experience. Geneva:
World Health Organization.

Comments
Post a Comment